How To Talk About Plus-Size Pregnancy Risks In A New Way
It's time to reframe how we talk about plus-size pregnancy risks.
When someone is trying to conceive or is newly pregnant, they're eager to have a deeper understanding of the risks they face during pregnancy. However, when you're plus-size, the information available is overwhelming, often confusing, and sometimes downright alarming!
From gestational diabetes and hypertension to preeclampsia, you scroll through article after article only to read all the scary increased risks associated with having a high Body Mass Index (BMI).
It's easy to question if it's even possible to have a healthy outcome during pregnancy in a larger body. People often feel broken before they’ve even begun!
The issue is, rarely do these articles explain how much of an increased risk people of size face. Instead, what you read is that you are at a “much greater risk,” which leaves you feeling discouraged and maybe afraid.
What’s more, these articles hardly ever provide details on how someone can reduce their risks during a plus-size pregnancy.
What if we talked about increased risks in a way that's empowering rather than frightening? What if we found a way to talk about plus-size pregnancy risks in a new way that is both hopeful and helpful?
High Risk Plus-Size Pregnancy
Before we dig into understanding plus-size pregnancy risks, we need to address a popular misconception.
People often assume they are having a high risk plus-size pregnancy.
While care providers set their own guidelines, the American College of Gynecologists and Obstetricians states that obesity is not an indication for the transfer of routine obstetric or gynecologic care.
If someone goes into pregnancy without any underlying medical concerns, they should receive individualized healthcare and not automatically be labeled high-risk because of their size.
Dr. Neel Shah goes into more depth on this topic during the podcast episode, Why We Need To Be Talking About Weight Stigma In Maternity Care.
Understanding Absolute Risk vs. Relative Risk
On the rare occasion when a resource shares numbers around risks, the information provided is almost always someone's relative risk.
Relative risk is a rate compared to another rate.
While telling a person with a BMI of 40 that they are four to five times more likely to develop gestational diabetes than someone with a BMI of 25 is accurate – it's not providing a complete picture. All you're doing is comparing one person's risk factor to another person's risk factor.
And it's easy to question, what does four to five times more likely mean? Is that 40% or 50%?
Absolute risk is someone's actual risk percentage.
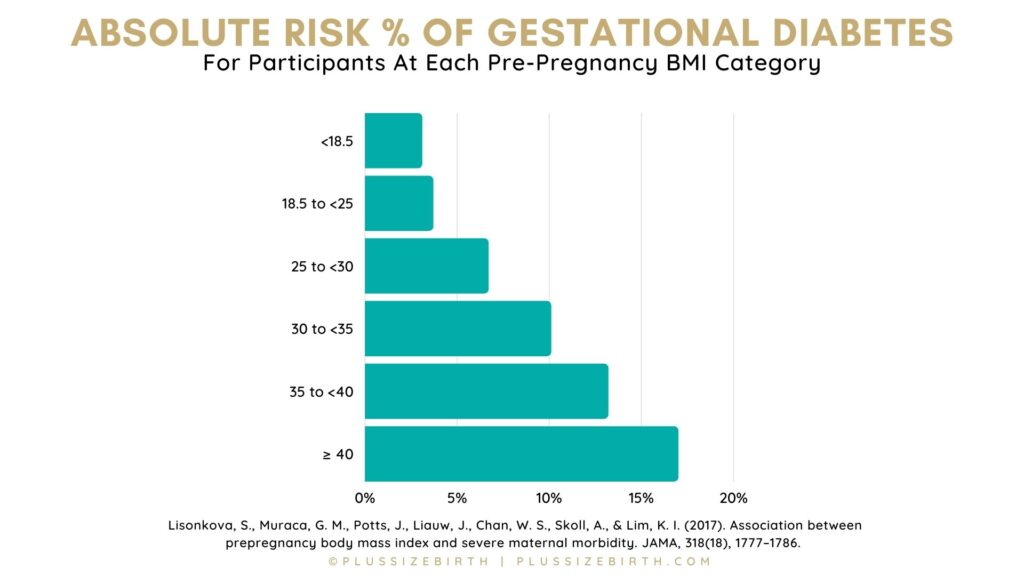
Let's break down the absolute risk of gestational diabetes during pregnancy based on BMI.
It's easy to see, yes, the risk goes up as someone's BMI increases.
Yet, the numbers are far lower than people tend to believe when they hear they are four to five times more likely to develop gestational diabetes (GD).
Someone's absolute risk percentage of incurring GD with a BMI over 40 is 17%.
That's nowhere near 50% or a guarantee this will happen to you!
See what a difference it makes when you know the absolute risk rather than only relative risk.
Unfortunately, it can be challenging to hunt down absolute risk numbers. Further, many studies available on obesity in pregnancy haven't excluded people who went into pregnancy already pre-diabetic or having high blood pressure.
So, more research is needed, but knowing the difference between relative risk and absolute risk is a great starting place.
How To Talk About Increased Pregnancy Risks
When someone hears the odds of having a healthy outcome are in their favor, they are motivated to focus on healthy habits that can further reduce their risks. Research on psychology and behavior change tells us that we’re more likely to make healthier choices over a longer period of time when the motivation for change isn't shame-based.
Above, we shared there's a 17% chance of incurring GD with a BMI over 40.
When you subtract 17% from 100%, you get 83%.
Imagine reading that you have an 83% chance of not incurring GD? How would that make you feel? Would you feel empowered to make choices working toward that 83%?
It's the same information, just reframed!
So, the next time you're reading an article about plus-size pregnancy risks, remind yourself that there are increased risks, but they are low. And if you're a birth professional, I hope you'll rethink how you discuss risks with your patients, and maybe even challenge your colleagues to do the same.
How To Reduce Plus-Size Pregnancy Risks
Along with sharing evidence-based information in a manner that's easier to understand, people should also be made aware of ways to reduce their risks.
When we look at all the risks people face during pregnancy, there's no one thing that only plus-size people incur. And as we've shown, while there are increased risks, they aren't as astronomical as people tend to believe.
During pregnancy, it's critical for people of all sizes to focus on nutrition, physical activity, and overall well-being. One other thing that makes a big difference is working with size-friendly care providers.

Nutrition
The American College of Obstetricians and Gynecologists (ACOG) recommends that plus-size people connect with a nutritionist during pregnancy. This is recommended both to reduce to risk of gestational diabetes and other complications but also to support both parent and baby with optimal nutrition for overall wellness!
Whenever possible, people should receive support from a Health At Every Size® (HAES®) aligned nutritionist. This way, they're working with someone who has addressed their size bias and is aware of the harmful impacts of diet culture.
To find a HAES®-aligned nutritionist, simply Google “HAES nutritionist” and your city. Other search terms are Health At Every Size dietitian, anti-diet nutritionist, and intuitive eating counselor.
Physical Activity
There are unique barriers people in larger bodies face when being physically active. Beyond the lack of plus-size maternity activewear, gyms are not always safe spaces for people with larger bodies.
Thankfully, community centers tend to be less fat-phobic and there have been a recent increase in gyms that are more friendly for bodies of all sizes. When in doubt, check it out! And trust your gut if the space doesn’t feel safe or accommodating for your body’s specific needs.
There are also many ways to be active during pregnancy that don't require a facility. There's something for people of all activity levels, from size-inclusive YouTube fitness videos to going for a walk. What's most important is finding an activity that brings joy!
Wellbeing
When it comes to health, we also need to talk about perinatal mental health! It's critical for people of all sizes to reduce stress and anxiety during pregnancy. Pregnancy is a great time to develop a new habit in a meditation or mindfulness practice.
You could try a meditation app or learn in a class or even just set aside a moment each day for some rest for your brain and body (so no phone!) – these habits will help your mental and physical health and set you up for a more peaceful parenting experience when the time comes.
And you guessed it; there are HAES®-aligned therapists and counselors too. If professional help to manage your stress and improve your mental health is necessary, be sure you find a great fit!
Size-Friendly Care Providers
While it's becoming easier to find HAES®-aligned nutritionists, therapists, and even size-friendly doulas, it's still challenging for people to connect with size-friendly medical care providers.
A size-friendly care provider is someone who provides evidence-based, compassionate care. They are aware of their size-bias and work to provide individualized healthcare.
These providers have the skills and equipment to support all of their patients.
It's shocking how often doctors tell people things that aren't evidence-based. A prime example is care providers telling women their vagina is too fat to give birth. This is also known as the fat vagina theory – yes, you read that correctly!
Unsurprisingly, plenty of studies show a care provider bias against people of size, making it even more critical that people connect with size-friendly care providers. We see improved outcomes for plus-size people and their babies when the medical professionals caring for them are size-friendly!
How To Find A Size-Friendly Care Provider
The hunt for size-inclusive care often begins with people reaching out to their plus-size friends. Many people have found it helpful to inquire about size-friendly OB-GYNs and midwives in local mom's groups on Facebook. This way, they can get recommendations of providers who live in their area.
Once someone gets a few names, they can do online research and read reviews. Then they can widdle down their prospective providers and book their first appointment.
It's important to ask questions to assess if a care provider is size-friendly or not. For example, one question is whether or not they classify people as high risk based only on their BMI.
It's also important to ask if there are any particular protocols or procedures patients should be aware of because of their size.
Here's a guide to connecting with a size-friendly care provider that goes well beyond the tips above.
But, ultimately, people need to trust their gut and be strong patient advocates.
Final Thoughts On Plus-Size Pregnancy Risks
By flipping the script on how we talk about plus-size pregnancy risks, we stop the spread of misinformation and empower people to be proactive with their health.
If your care provider keeps telling you that you're “X” times more likely to develop something, ask them for your absolute risk. Just don't be surprised if they don't have an answer!
You deserve a care provider who helps you feel empowered about your odds of having a healthy outcome during pregnancy! It’s not only possible, it’s probable!
Reference
Lisonkova, S., Muraca, G. M., Potts, J., Liauw, J., Chan, W. S., Skoll, A., & Lim, K. I. (2017). Association between prepregnancy body mass index and severe maternal morbidity. JAMA, 318(18), 1777–1786.
- Will My Baby Bump Show if I'm Overweight? - September 14, 2025
- Plus Size Maternity Pose Guide: 25+ Confidence-Boosting Poses - May 26, 2025
- Plus Size Pregnancy Confessions: We Listen and We Don't Judge - December 15, 2024








I cannot begin to tell you how much I have needed this! I pregnant with our first baby and 2 out the 3 doctors I have seen have been absolutely ugly about my size. By the BMI chart I’m 36%, but I am healthy across the board for everything, no high blood pressure or high blood sugar. I eat right, excercise, and even check my blood pressure a few times a week. It’s ridiculous that we know bmi is not a true indicator of health but they still scrutinize and traumatize women on their weight. Keep fighting the good fight, and let’s educate people on how to advocate and care for themselves!