Plus Size Labor And Delivery – 11 Things You Need To Know
You've landed here because you're researching plus size labor and delivery. Whether you're curious about options for plus size labor and delivery gowns or searching for evidence-based information to help prepare for childbirth – you're in the right spot!
Below we're sharing eleven things you should know before giving birth in a larger body.
Disclosure: Plus Size Birth is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program. As an Amazon Associate, I earn from qualifying purchases. Read more about these links in my disclosure policy.
1. Be Aware of BMI Restrictions
Long before you're in labor, you should be aware of any BMI restrictions if you're giving birth in a medical facility.
Some hospitals have BMI limits for a water birth or access to midwifery support. In addition, some hospitals have attached birthing centers but have a BMI cut-off for their use.
Most free-standing birth centers have BMI limits. And those that don't will sometimes allow you to labor in a birthing tub. However, you may need to get out of the water to give birth due to other restrictions.
Along with BMI restrictions, you'll want to ask if your selected facility has any routine protocols for people of size. Remember that you have the right to refuse any interventions. But when protocols are in place, it often feels like you don't have a choice.
So, find out if there are any BMI restrictions or protocols well in advance. That way, you'll know what to expect when it's time for you to give birth.
2. You Can Wear Whatever You Want During Your Plus Size Labor And Delivery
You have options around what to wear when you're in labor. The same goes for giving birth unless you have a cesarean delivery. In that case, you'll wear a hospital gown.
Hospital Gowns
Most facilities offer regular and bariatric size labor gowns.
Your Clothes
You don't have to wear a hospital gown!
As long as your care team has the access they need for monitoring, you can wear whatever you want. And the same goes for birth aside from a cesarean delivery when you'll likely need to wear a hospital gown.
Some people like wearing a sports bra with a skirt and they sometimes also wear a robe. While others wear nothing at all!
It's entirely up to your comfort level. And there’s sure nothing wrong with wearing what the hospital provides – including the fancy mesh underwear.
Speaking of mesh undies, they come in different sizes. You can always ask if there's a larger size available. Or you can even purchase your own in advance.
Plus Size Labor and Delivery Gowns
Plus size labor and delivery gowns are becoming more and more popular!
You can pick up a plus size labor gown from Motherhood Maternity, Etsy, Amazon, and Dressed To Deliver.

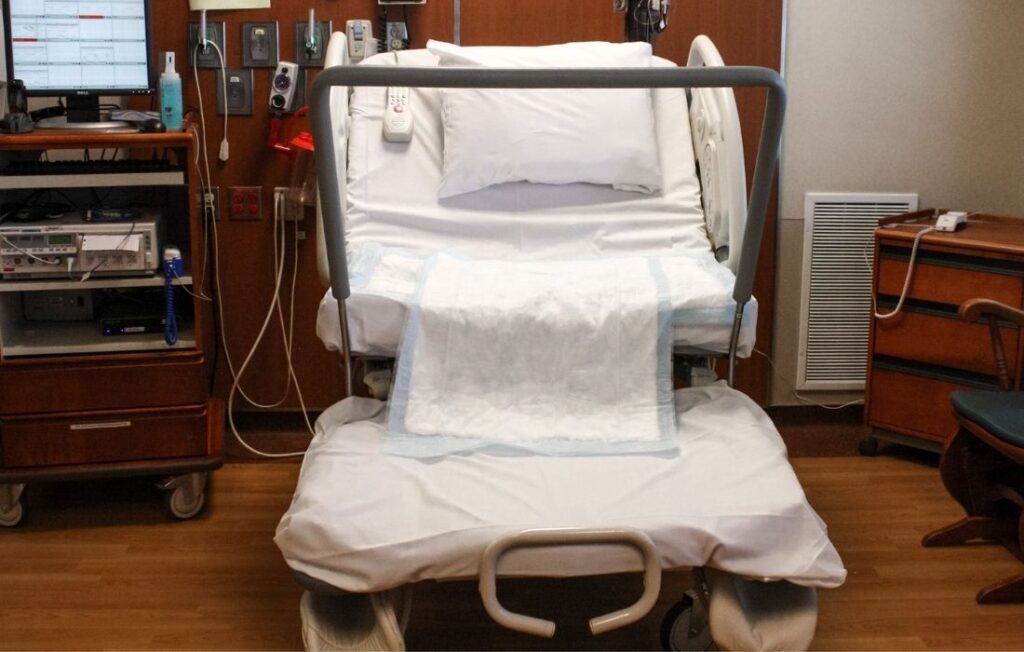
3. Hospital Bed Weight Limits
Some facilities have bariatric labor and delivery units. However, they aren't necessary for most people giving birth with a high BMI.
It might put your mind at ease to know standard labor and delivery beds have a weight limit of 500 lbs and 400 lbs for the foot section.
4. Monitoring During Labor
Monitoring contractions and your baby's heart tones can be harder for people in larger bodies. There's nothing wrong with your body – most of the technology used today wasn't designed with plus size bodies in mind.
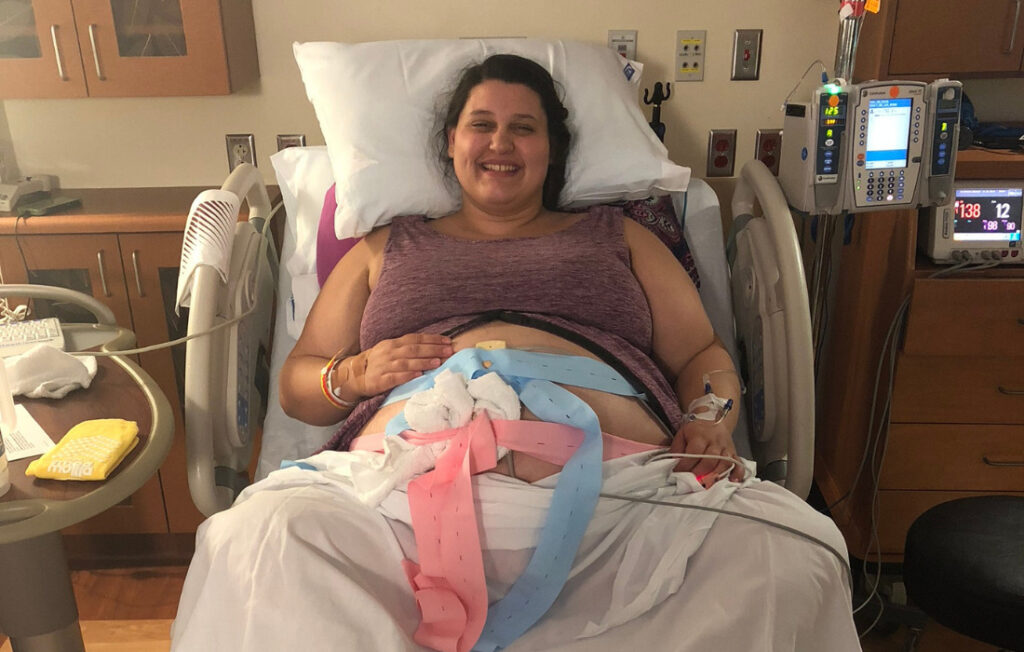
External fetal monitors, with one strap holding a monitor in place to pick up your baby's heart rate, and the other picking up your contractions, don't work as well on plus size bodies for a few different reasons.
Due to your belly shape, it might be harder to place the monitors, and it's also more challenging for the doppler-based fetal monitor to pick up the baby’s heart rate through your tissue.
Many find bringing a belly band from home (that they know fits well) helps to hold the monitors in place.
You can also use rolled-up washcloths to help hold the monitors in place (see the photo below). Your labor and delivery nurse will probably also suggest a few other helpful tricks.
Wireless monitors, especially the Novii Wireless Patch System, tend to work better for people with a high BMI.
The Novii system was explicitly designed for those with a high BMI. Still, it's not available at all medical facilities, so be sure to inquire if yours carries this wireless monitor.
Intermittent monitoring with a handheld doppler ultrasound is preferable for low-risk people (and you can be low-risk and have a high BMI). However, if your labor is induced, you need Pitocin, are having Vaginal Birth After a Cesarean, or if you'd like an epidural, you'll receive continuous fetal monitoring.
Sometimes plus size patients feel pressured to consent to internal fetal monitoring. This is the case especially if the external monitors cannot continually monitor the baby's heart rate and/or your contractions without being routinely adjusted.
For internal fetal monitoring, your bag of waters must be broken. This type of monitoring comes with increased risks, so be sure to do your research, but know it might become necessary.
Some people prefer internal fetal monitoring because their care team doesn't have to fuss with the external monitors constantly and this can give you more mobility.
Please note that even with continuous monitoring, your care team should be able to help you move positions frequently. Consider adding a note in your birth plan about wanting help moving positions 1-2 times every hour, even if you have an epidural. This can really help with labor progression.
5. You Might Have An Early Consult with an Anesthesiologist
The American College of Gynecologists and Obstetricians (ACOG) recommends an early consultation with an anesthesiologist for people with a high BMI.
This may or may not occur for you, but it's something to be aware of as you'll want an anesthesiologist skilled with supporting people in larger bodies if you have an epidural or cesarean birth.
Epidural placement can be challenging due to adipose tissue (body fat), making it harder to find landmarks for positioning. So, if the person placing your epidural is having great difficulty, you can inquire if there's someone else on staff who can support your needs as a plus size person.
Rest assured that a skilled anesthesiologist can place an epidural for people weighing over 400 lb.
If possible, have a doula or support person there during placement to provide you with much-needed emotional support and encouragement.
6. You Need More Time To Labor
The first stage of labor often takes longer when you have a high BMI. So be sure to advocate for extra time during labor if your care provider starts talking about you needing a c-section due to failure to progress.
During pregnancy, Spinning Babies is an excellent resource for helping to get and keep your baby in the optimal position for birth.
When it comes to labor, it’s important to change positions about every 30 minutes to keep things progressing. When you move while receiving continuous fetal monitoring, the monitors will also likely need to be adjusted. So, hopefully, you can work as a team with the labor and delivery nursing staff on this whole process.
This is one reason to try and hold off as long as possible before consenting to interventions that can slow down the progression of labor. With that said, even if you want an epidural, you can still get into different positions during labor to keep things progressing.
If you have a support person, like a doula, ask how they can also assist with supporting changing positions and keeping the monitors in place.
For an unmedicated low-risk labor, you'll have a lot of freedom of movement with intermittent monitoring. And hopefully, you’ll have access to hydrotherapy with a shower or tub.
The labor and delivery bed can adjust in many ways, including having a squat bar added to get into different positions. In addition, some people like using a peanut ball or birth ball to get into different positions if restricted to the bed.
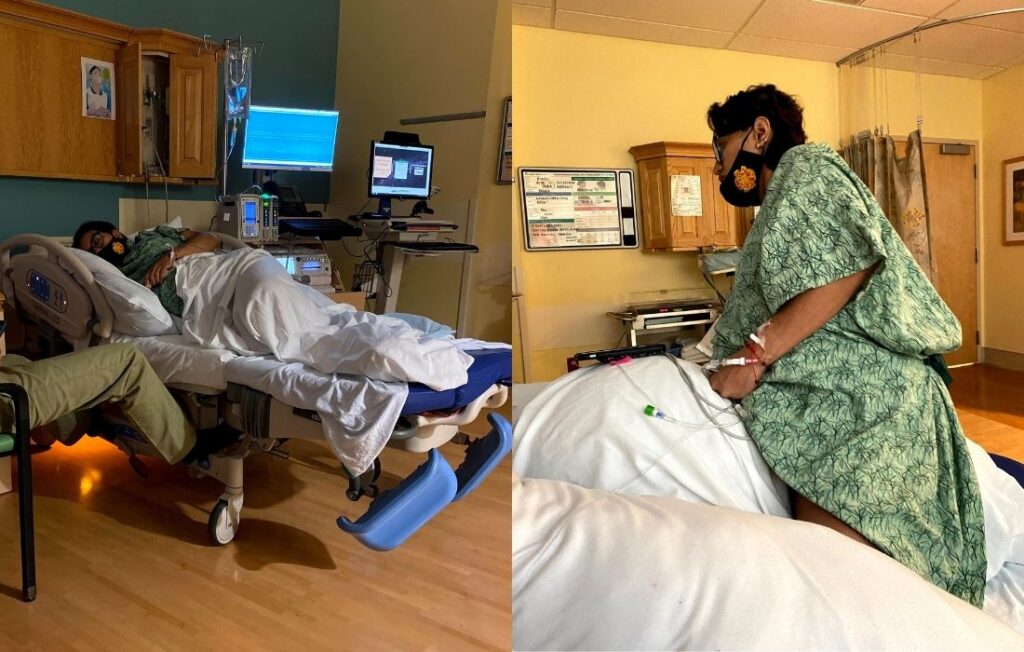
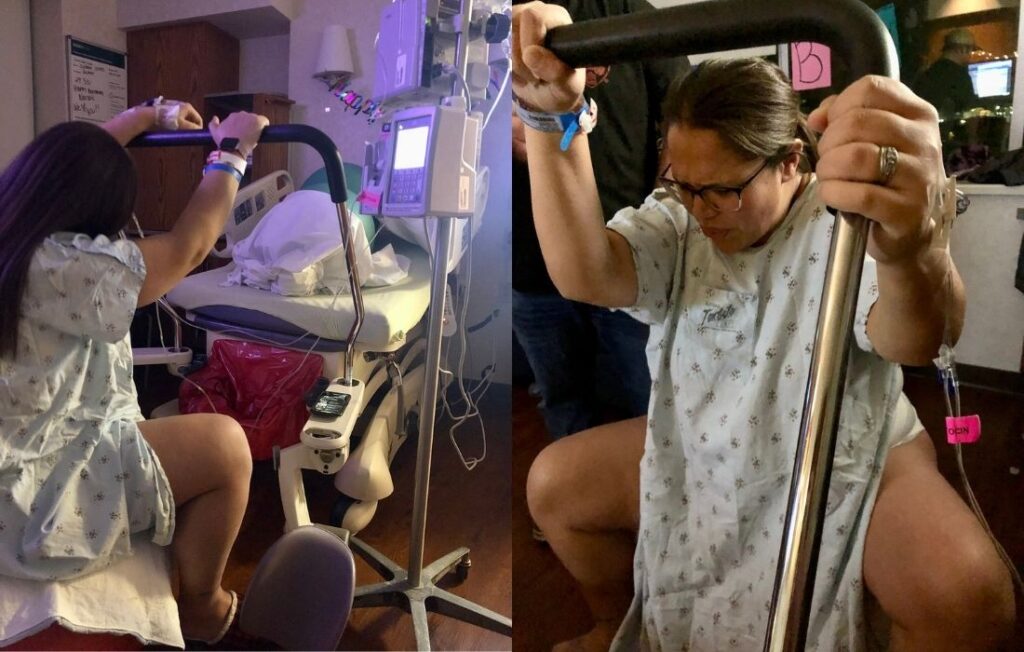
7. Pushing Positions Plus Size Labor And Delivery
During labor, you'll want the freedom to move as your body directs, and the same goes for the second stage of labor: pushing!
While you might've heard some of the biases against plus size women in labor, including being told their vagina is too fat to give birth, studies show these myths are simply not true!
While the first stage is often longer as your body dilates, the second stage of labor tends to be shorter for people with a high BMI!
You'll want to continue to try different positions while pushing to keep things moving along.
If you have an epidural, the side-lying position can be beneficial. Peanut balls are great tools to help with positioning.
You can ask to have the squat bar set up on the bed as well if that would be helpful.
Beyond using the squat bar to lean against for different positions, you can wrap a sheet onto it to play tug-of-war while pushing to help you bear down.
A kneeling position on the bed can be an effective pushing position, with the hospital bed's top part raised for people to lean against. You're also using gravity with this upright position to help bring your baby down.
Listen to your body, follow the suggestions of your care team, and keep trying different pushing positions.
8. Birth Positions for Larger Bodies
Most care providers will “allow” people to get into multiple positions for pushing but ask you to be on your back to give birth. You're not lying flat on your back in this position though, it’s more of a semi-recline.
The nursing staff will help support your legs, and you may use the stirrups as you see in the movies, but not always.
When nurses and loved ones hold someone's legs, sometimes they are pulled too wide, or keens become pushed too far up. This can cause joint hypermobility, leading to possible hip, lower back, and nerve issues. So, if you're pushed beyond your normal range of motion, be sure to voice any discomfort. And have your support team lookout for this, especially if you're planning to have an epidural.
We've described the lithotomy position above, and it's the typical position in which people of all sizes give birth. It's one of the most accessible positions for care providers to support you but it’s not actually the most effective position for giving birth.
So, be sure to speak with your care provider about what positions they support for birth during your prenatal visits. And if your selected care provider isn't present for your birth, make sure your wishes are known early on by voicing them to the nursing staff and the provider who attends your delivery. As well as making sure your wishes are listed in your birth plan!
Some providers are okay with people giving birth in side-lying positions, which can be good for plus-sized people.
If you're having an unmedicated labor or your epidural isn’t too strong, you may be able to get onto all-fours or a forward-leaning kneeling position on the bed. This position tends to be great for plus size people who don't have any knee problems.
For home birth, birth center birth, and even some hospitals, water birth is a popular option. It allows for excellent freedom of movement and the ability to get into multiple positions, thanks to buoyancy. However, some facilities have BMI restrictions for a water birth, so be sure to inquire about this if it’s of interest to you.
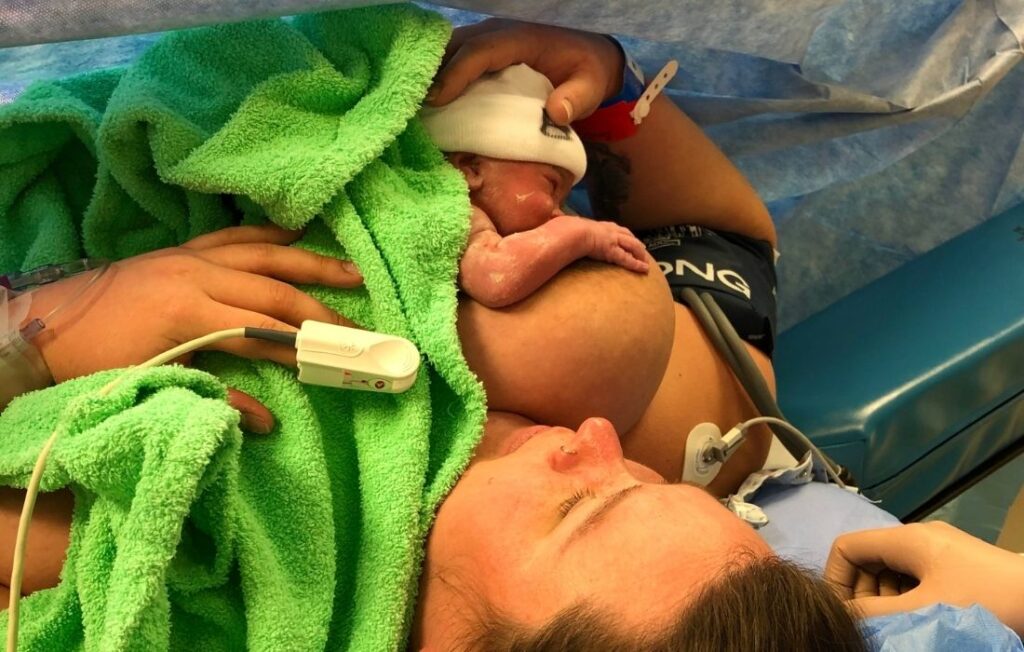
9. Cesarean Birth with a High BMI
Having a cesarean birth when you're plus size looks a little different than for someone who’s smaller.
Don't worry about being lifted and moved onto the operating table, as your care team is skilled at moving people of most sizes. In addition, many operating rooms have a special mat that inflates to help move people.
When preparing your body for a cesarean birth, your care provider needs a clear and visible area to make their incision. Therefore, they will need to lift your belly out of the way (especially if you have an apron belly. Most facilities now use a panniculus retractor (which looks a lot like plastic wrap), but some still use tape to hold your stomach up.
Having your stomach tugged on and moved out of the way shouldn't be painful, but it can be emotionally distressing. So, take some deep breaths and remember you're about to meet your baby.
If it helps to have the care team talk you through what is happening, you can ask for that. Or you might prefer having your support person distract you with a story or jokes or looking at photos of your dog or anything else that makes you happy!
When you have a BMI over 30, there are some increased risks for having a cesarean birth, including longer operating time and a greater risk of infection, so be sure to follow all after-care instructions closely. And as soon as you're able, get up and start walking (with support from your care team) to promote healthy blood flow and healing.
A wound vacuum is something plus size women have found helpful when recovering from a c-section. However, some research shows it does not result in a significant reduction in wound infections. So, inquire with your care provider if you’re interested in learning more.
We have an extensive resource for having a cesarean birth with a high BMI with more information and helpful tips.
When it comes to having a Vaginal Birth After Cesarean (VBAC), you'll want to make sure you've connected with a care provider who is not only size-friendly but also VBAC-friendly.
You can read inspiring VBAC stories from plus size women to hear different experiences to help you prepare. We also have this podcast interview where we learned a lot on the subject.
10. How To Advocate For Yourself
Unless there is a true medical emergency for you or your baby, there should be time to get all of your questions answered before you consent to a medical procedure during your plus size labor and delivery.
The BRAIN acronym is a helpful set of questions that help you fully understand what your care provider is recommending and why.
BRAIN Acronym
B – What are the benefits?
R – What are the risks?
A – What are the alternatives?
I – Always listen to your intuition!
N – What happens next or if we do nothing?
You might also want to consider hiring a doula as they will support you not only throughout your labor and birth but help you to know about all of your options well in advance. See our list of size-friendly doulas!
Your nurse will spend far more time with you throughout your labor than your family doctor, OB-GYN, or midwife. Commonly, you'll experience a few shift changes throughout your labor, so you likely won't be with the same nurse the entire time.
The way this process unfolds leads to unfamiliar hands helping you, sometimes every few hours. We hope you don't incur any mistreatment due to your size, but unfortunately, it sometimes happens.
If at any point you feel your nurse is shaming you because of your size or is not equipped to support a plus size patient, you can ask to speak with the Charge Nurse. Then, address your concerns and see if another nurse who is more size-friendly is available to provide your care. If you have a doula, they can also help you with this or you can ask your partner to help advocate for you to get better care.
Your options for switching care providers might be more limited, but that shouldn't prevent you from speaking up if you're feeling uncomfortable.
Labor And Delivery Nurses Speak Up
Listen to labor and delivery nurses speak frankly about the treatment plus size people receive during episodes of the Plus Mommy podcast. These nurses also give self-advocacy tips you don’t want to miss!
- A Labor And Delivery Nurse Talks About Failing Plus Size Moms
- Plus Size Labor And Delivery – Everything You Need To Know
- Supporting Plus Size Labor And Delivery With Mommy Labor Nurse
11. Your Body is Amazing!
We’re closing this list with our recommended items to pack in your hospital bag which includes lots of self-care items to tend to your incredible body.
We hope you've found all of these plus size labor and delivery tips helpful.
You've come so far, growing life within you, and now it's time to prepare for your upcoming birth. We want to end with a reminder that your body is amazing: worthy of love, patience, compassion, and adoration.
You've got this!
Plus Size Labor And Delivery References
- Paladini, D. (2009), Sonography in obese and overweight pregnant women: clinical, medicolegal and technical issues. Ultrasound Obstet Gynecol, 33: 720-729.
- ACOG Committee opinion no. 549: Obesity in pregnancy
- Hanne Jensen, AndersOle Agger & KjeldLeisgaard Rasmussen (1999) The influence of prepregnancy body mass index on labor complications, Acta Obstetricia et Gynecologica Scandinavica, 78:9, 799-802
- Shayna M. Norman, MD, Methodius G. Tuuli, MD, MPH, Anthony O. Odibo, MD, MSCE, Aaron B. Caughey, MD, PhD, Kimberly A. Roehl, MPH, and Alison G. Cahill, MD, MSCI. (2012) The effects of obesity on the first stage of labor. Obstet Gynecol. Jul; 120(1): 130–135.
- Chu, S.Y., Kim, S.Y., Schmid, C.H., Dietz, P.M., Callaghan, W.M., Lau, J. and Curtis, K.M. (2007), Maternal obesity and risk of cesarean delivery: a meta-analysis. Obesity Reviews, 8: 385-394
- Will My Baby Bump Show if I'm Overweight? - September 14, 2025
- Plus Size Maternity Pose Guide: 25+ Confidence-Boosting Poses - May 26, 2025
- Plus Size Pregnancy Confessions: We Listen and We Don't Judge - December 15, 2024
















Thank you so much. Very informative.
I was told at 16wks that the hospital I intended to deliver at recently changed BMI guidance and would not allow me to deliver. I had to switch not only to a new hospital but also a new practice that delivered at the much larger, university hospital. I strongly encourage newly expecting moms to ask your OB if your intended delivery hospital has any BMI restrictions! This caused a lot of anxiety and shame for me not finding out until 16weeks along.