A Single Umbilical Artery Pregnancy Story
This is Julie's story of having a single umbilical artery pregnancy.
She shares the uncertainty that comes with having unexpected complications during pregnancy and birth.
Single Umbilical Artery Stories
Single umbilical artery stories are helpful to read following a diagnosis. While this is just one story below, you can find others who have shared their experiences via Google. There are also some Facebook support groups!
Pregnancy Story
I found out I was pregnant in June of 2016.
It was no surprise since we had been planning, tracking, monitoring and logging my temperature for months.
My due date was Feb 18th.
Note that I am plus sized and would be turning 35 before the baby was born, so high-risk status was on the table. Add to that that both of my parents are diabetic and I was a hat-trick for a full intervention childbirth.
However, I had a plan.
I would do what was needed to have as natural a childbirth as possible, but be open to whatever was needed to keep me and my baby safe and healthy.
That meant good diet, continuing my 2-3 days per week habit at Curves, and getting the education I needed to have a healthy pregnancy, natural birth, and successful breastfeeding journey.
My doctor told me early on that a cesarean was likely for me, but I was going to try whatever I could to avoid one.
My pregnancy was very easy. To the point that it made everyone I spoke to about it either jealous or angry. They felt this way for all the suffering they or their wives had endured during their own pregnancies.
I had no morning sickness other than some mild motion sickness one weekend on a trip up a curvy mountain.
I had no swelling. No cravings. A couple food aversions. Minimal weight gain.
I'm 6′ 1″, so my long torso made a great, non-squished fort for my baby to grow in with no lung or breathing impact to mama.
The worst I had was circular tendon aches that made me take a few extra seconds to relax and stretch before walking to the bathroom for my early morning preggo pee. Also, a bit of heartburn that I mainly controlled through diet.
At my 18 week ultrasound, we found out we were having a little boy.
We also found out that he had a two-vessel cord or single umbilical artery (SUA).
Needless to say, you're never prepared to hear that there is something wrong with your kid. Even with reassurances from the doctor that it was reasonably common and most babies have no impact as a result when having a single umbilical artery pregnancy, your mind still spins and the fears seep in.
Most babies are fine, but 25% could have heart or kidney defects.
The babies could have intrauterine growth restriction or even fetal demise.
The news, our son having single umbilical artery pregnancy, cast a shadow of uncertainty over what should have been a giddy, happy, excited time preparing for the arrival of our first child.
After a few days of consulting Dr. Google, I found that worrying wouldn't do any good. We would hope for the best, plan for the worst, and take it day by day.
Next concern? Gestational diabetes (GD).
With the husband being diabetic, I already ate low carb, high protein. Add the Brewer diet instructions from our Bradley class and a trip to Curves 2-3 times a week and I had the best chance at avoiding GD.
Luckily, I passed glucose challenge tests with flying colors.
Next concern?
Mental state. I needed the knowledge of what possibilities were ahead and needed to eliminate any fear or anxiety from the process.
Our Bradley class took care of most of that. We learned anatomy, nutrition, stages of labor, relaxation, standard procedures for natural and assisted childbirth, complications and interventions, breastfeeding, and some postpartum care for mom and baby.
I supplemented that with lots of pregnancy podcasts as well as Ina May Gaskin's Guide to Breastfeeding.
We were as ready as we were going to be.
I started having routine non-stress tests (NST) at week 32.
Given my plus sized pooch and the baby's desire to either do somersaults or play the roll of bump on a log, the monitoring was difficult.
I had to be laying flat on my back for long periods of time and I had to drink ice water to entice some accelerations from the kid. I was even sent to the hospital for additional monitoring once when the kid wasn't cooperating.
We had a birth plan… to go as natural as reasonable, but be open to interventions if necessary.
No IV, external intermittent monitoring, no epidural, no Pitocin, no cesarean.
The difficult NSTs were a definite foreshadowing of what was to come. My doctor recommended induction at 39 weeks to minimize any complications with the SUA.
We now had a hard date of Saturday, Feb 11th to be admitted to the hospital.
Starting the week before, we intended to try some natural induction techniques, but Murphy's law intervened and my husband got a severe respiratory infection.
So much for the fun stuff. I was left to walking, going to the gym, and a membrane sweep by the doctor. I was 2cm and the baby was low on Thursday. Looking good.
Birth Story
Our check-in time was 10 pm on Saturday, but that got bumped to 1 am with how busy the hospital was. My sister, my husband and I got shown to our room and got all the initial monitoring done. Still 2 cm.
I got a dose of Cytotec to help soften my cervix and start the contractions.
To avoid the IV, I was snacking and hydrating regularly.
I walked the halls every couple hours and had lots of pee breaks. When I wasn't walking, I was lying on my back being monitored, which sucked.
Back pain, an uncooperative baby who was dancing in the womb, and no ability to assist in helping labor progress made for a miserable morning.
My nurse called my doctor and they recommended breaking my water to help kickstart labor.
As well as to put a monitor on the baby's head to get consistent monitoring.
My doctor arrived before noon and used a tool very much like a crochet hook to break my bag of waters.
Turns out there was meconium in the water. Baby had pooped at some point, which meant NICU had to be on site for delivery to evaluate the baby.
I was 4 cm and the baby's head was further down.
My doctor inserted the internal monitor and the nurse setup my catheter and we were rolling.
Come mid-afternoon, I was 5 cm. The contractions were much stronger and I was not handling them well. I was strapped to a bed. So other than breathing techniques, there was nothing I could do to help cope with and progress my labor.
I started clenching the bed rails and crying uncontrollably while breathing through some bad contractions. I decided an epidural was in my future. 30-45 minutes later I was drugged and feeling so much better. Happy tinglies in the legs, no contraction pain, and a strong desire to sleep.
As expected my labor slowed, so the Pitocin was set up.
Come at 10 pm, I was 8 cm and starting to feel contraction pain again. My epidural was boosted and my left leg went completely numb. Right leg was still able to dance. 3 am, 9.5cm and everyone was napping as best we could in the oh-so-uncomfortable bed and chairs in my room.
Then the chaos began.
At 5:30 am the nurse walked in, turned on all the lights, jarring everyone awake, and said that we were having this baby by 6:30 am. The bed was broken down, everything was moved away from the bed, the doctor was called, NICU was summoned, and by 5:40 am I was pushing.
Needless to say, both my husband and my sister were surprised when the nurse told them each to grab a leg.
They were going to be delivering this baby! I was sat at an upright angle, knees pulled up and back, and the counting cycles of breathing began with each contraction.
At 6:07 am, my son was born.

He was placed on me for a quick hi and hello, then reviewed by the NICU staff.
APGAR was 8 & 9 and he hadn't aspirated any meconium.
No one had informed the NICU staff that the baby had a single umbilical artery, so there were a few tense moments while everyone got on the same page. My doc was stitching up my 2nd-degree tear, and I was getting to know my son.
Bright-eyed and squishy, all 8lb 5oz, 20 inches long of him.
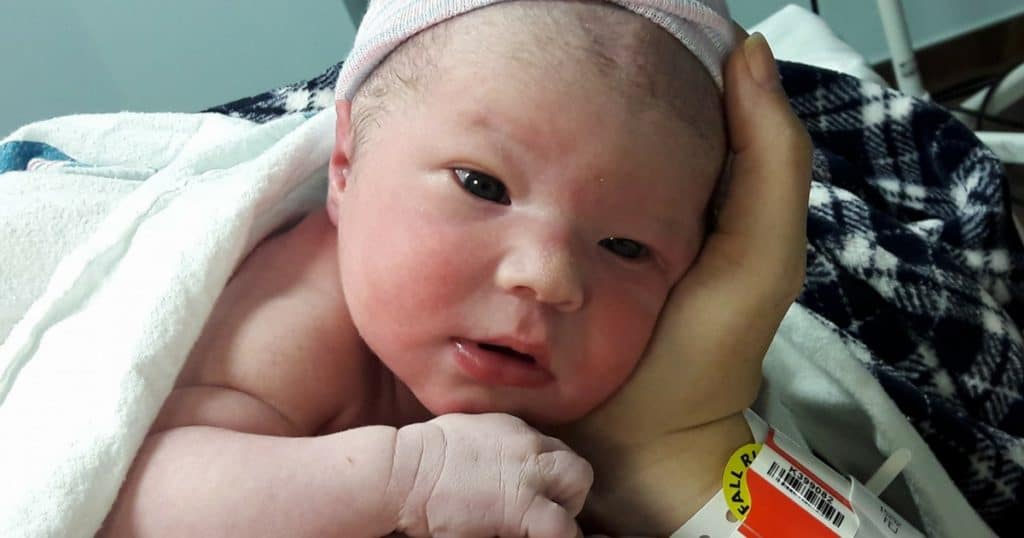
He latched great and was calm and snuggly right away.
After doing skin-to-skin for about 20 minutes, I asked Daddy if he wanted to hold the baby and his eyes lit up.
He ripped his shirt open and reached for the kid as fast as he could.
I had been somewhat disconnected for my whole pregnancy and labor. Seeing Brian hold our child with such love and happiness and protection and sheer joy finally melted my stone-cold heart.
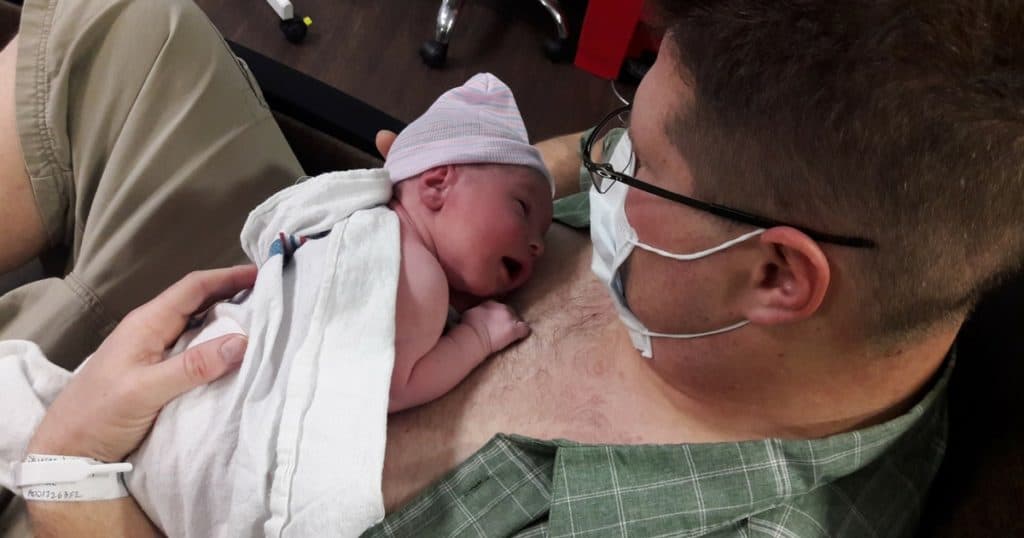
We spent a day and a half recovering in the hospital then went home to enjoy three weeks of hell.
Jaundice off the charts, a lip and tongue tie which affected milk transfer, failure to thrive, projectile vomiting of the supplemental formula, and a diagnosis of reflux requiring meds made the early bonding time very stressful. But we had a village!
My sister, Father-in-Law, and Stepmom stayed with us throughout the first month. They each cooked while they were with us.
We ended up with a month of food from family and friends in the freezers once we were finally on our own.
James is loved by so many. I can't wait to see the young man that our village produces!!!!
Read even more plus size birth stories!
- Will My Baby Bump Show if I'm Overweight? - September 14, 2025
- Plus Size Maternity Pose Guide: 25+ Confidence-Boosting Poses - May 26, 2025
- Plus Size Pregnancy Confessions: We Listen and We Don't Judge - December 15, 2024









I was just diagnosed with a SUA and your post made me feel a lot better (despite your 3 weeks of hell!) Thanks for sharing your story!
I’m so glad this story helped you to feel less alone!