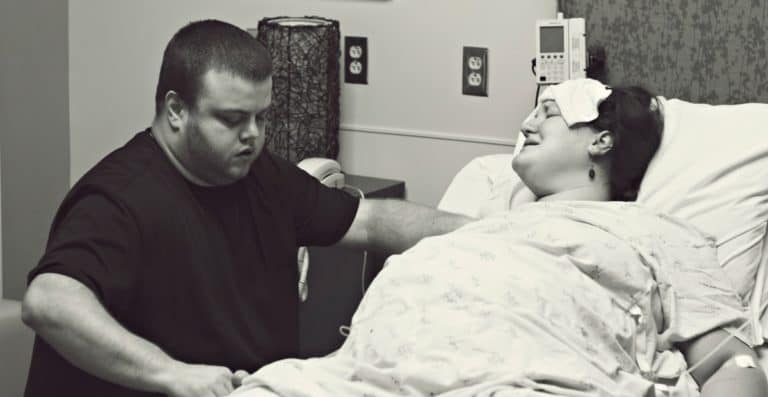
A Fight For My Plus Size Natural Birth
For many desiring a plus size natural birth, it can be challenging to connect with a supportive size-friendly care provider. This is one mom's story…
My Plus Size Natural Birth
At 24, I probably should have felt much more prepared to see those two blue lines indicating “positive” than I would have if my husband, Don, and I were still dating teenagers instead of working adults. But as I lowered my head between my knees to prevent myself from blacking out, all I could think was “I’m not ready.”
We talked through different options. Yet, I don’t think there was ever truly a question that, ready or not, we were bringing a child into the world.
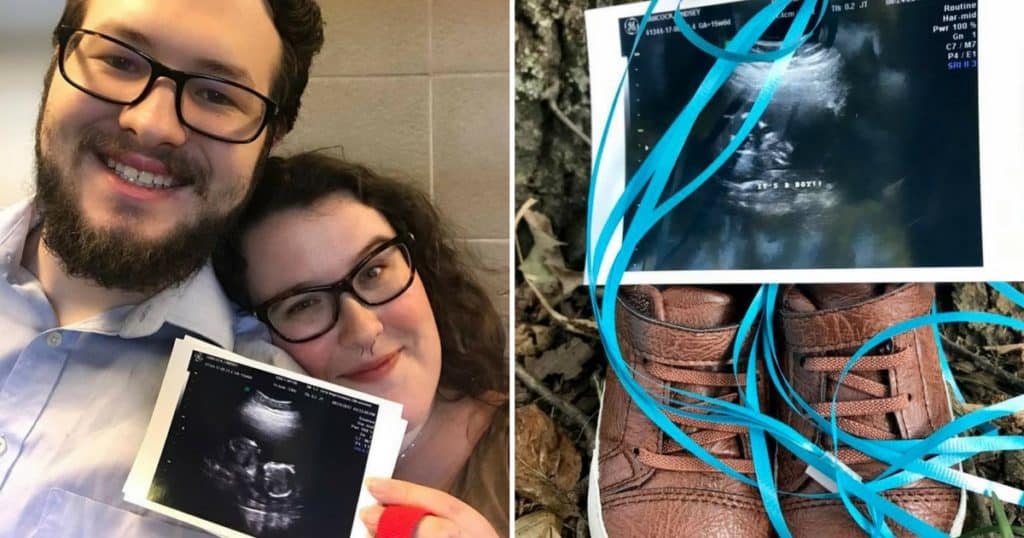
During our elective gender scan, we were shocked to learn we were welcoming a baby boy. I had insisted since we found out that it would be a girl. Just the first of many curveballs and surprises along the way.
It turns out that your body and your baby have an agenda all their own.
It was not the easiest pregnancy, especially for a control freak like me. My morning sickness prevented me from doing anything but laying in bed with a fan on my face for days at a time.
By the second trimester, it felt like the baby was living in my ribcage. The pain would get so bad by the end of my workday that I would come home and go straight to the couch or the bed.
I fell right before Christmas, tearing a tendon, and spent the majority of the next two months in an orthopedic boot.
Related: Yoga for Back and Hip Pain During Pregnancy
Needless to say, I was ready for things to start going my way again. That’s why I wrote out a detailed birth plan wanted to try for a vaginal delivery with no epidural or major interventions.
I never liked the idea of being confined to the bed. I have been afraid of needles all my life and had an inkling that I might not want to push while laying on my back.
When my OB/GYN provider suggested that I should be open to the possibility of induced labor or a c-section, both of which are almost considered standard interventions in our area, Don and I decided to make a change.
We were very nearly in the third trimester when we switched practices to a group of midwives who deliver at our local regional hospital and tout more personalized care.
We went over my birth plan, and they said it looked good. I tried to project confidence, telling them that my mom went early with all three of her babies and that I would probably be the same. I put in for maternity leave at work, though I was mentally prepared to go out early.

The first wrench in the plan I had laid out in my mind was that my midwives asked me about two months out to start undergoing fetal non-stress test scans at their partner high-risk clinic once a week.
I was so confused. My blood pressure had been beautiful the whole pregnancy. My gestational diabetes test results had come back far under range.
When we asked in the office what about my pregnancy was considered “high-risk,” the midwife we were speaking with explained that it was hospital policy for me to undergo the scans because of my higher BMI.
She went on to explain scary terms like “spontaneous fetal death,” “increased risk of birth defects,” and “emergency cesarean.” She said I could refuse the non-stress tests if I wanted to, but made it sound like I was putting myself and my baby at risk if I did.
I waffled between anger, confusion, and guilt.
It felt like my body wasn’t healthy enough to safely carry and deliver my baby.
Feeling discouraged, I decided to agree to the additional level of tests and tried to just consider it an extra layer of care for Baby. Thankfully, we passed each non-stress test (NST) with flying colors.
As we approached the two-weeks-from-due-date mark, I was feeling good and assumed I could go into labor at any time.
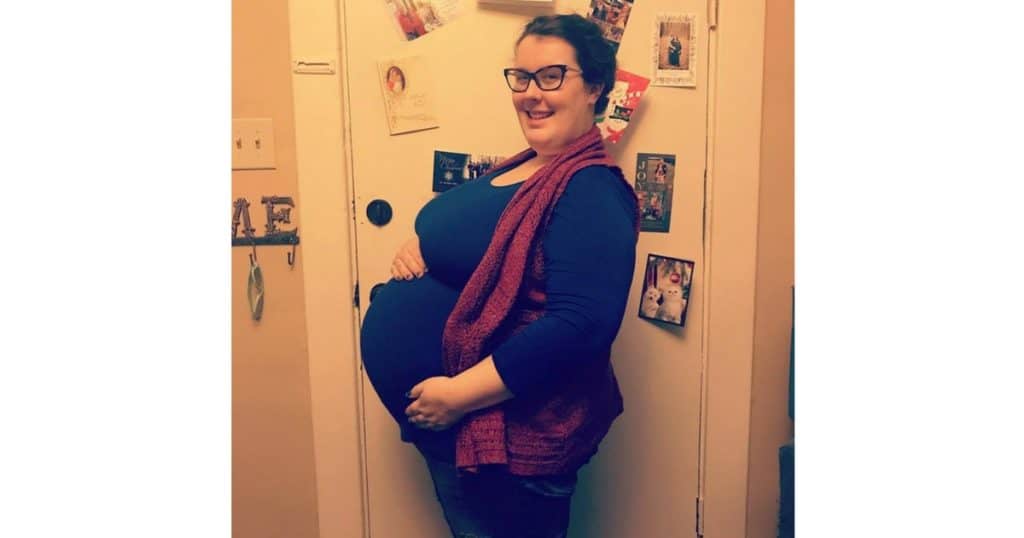
I had Braxton-Hicks contractions throughout the pregnancy. On a particular Wednesday, that I was also scheduled for an NST, I felt like I was starting to feel more intense contractions. Sure enough, the contractions also showed up on the doctor’s monitor. They decided to check my cervical dilation, but I was only dilated to one centimeter.
Feeling like baby’s birthday could still happen anytime now, Don and I anxiously awaited any sign of regular contractions. I continued working, feeling contractions throughout the workday as well as a new symptom of pelvic pressure.
Related: What My Obese Pregnancy Taught Me About My Body
On Friday the week following my NST, Don and I started timing what seemed like regular contractions. They were about four and a half minutes apart.
While I could still walk and talk through them, we decided to go into labor and delivery at the hospital and get things checked out.
A kindly nurse, after monitoring the baby and checking his positioning, explained that the baby was positioned posterior in my uterus. This meant that, although he was head down, his back was facing my back instead of the other way around.
She told me that while my contractions were real, I was experiencing what they call “prodromal labor.” It mimics true labor and can go on for days or weeks. They told me to try to spend some time on all fours to help the baby get into a better position.
My due date came and went.
I cleaned my house. Don and I went to IKEA and walked around for hours. I ate spicy food. All of these things seemed to intensify my near-constant prodromal contractions, but they would always peter out after a few hours. My midwifery team suggested a chiropractor, who adjusted my pelvis and tailbone to try to help Baby drop.
Though my midwifery team had not suggested an induction or a scheduled c-section, some of my family members started suggesting it.
When a midwife asked how I was doing at an appointment, I burst into tears and told her through massive sobs that I was just so UNCOMFORTABLE. I was growing concerned that my baby was growing too big for me to birth. They were not doing weight estimates on my baby via ultrasound. I had gained ten pounds in two weeks and was just sure that the baby was getting huge, too.
It was a very discouraging point in my pregnancy.
On the Monday before baby’s birthday, Don and I ran some errands and went to another scheduled NST at the high-risk clinic. We got home around 5:20, and Don went to class. I soaked in the bathtub for an hour or two.
The bath was my go-to throughout pregnancy to relieve stress, tension, and pain. I also did poses from a set called the Miles Circuit, which is supposed to help posterior babies flip and bring on labor. By the end of the Miles Circuit set, my contractions were back and I was feeling pretty good.
Don was back from class, and since he works nights, we decided to go to bed early. By 11:30, my contractions had grown uncomfortable enough to keep me awake. Don left for work, but I warned him that I may need to call him to come home.
By two in the morning, I was still far too uncomfortable to have gotten any sleep and my contractions were getting worse. I decided to get back into the bathtub, where I planned to spend most of my early labor. I called Don to come home from work.
The bath did not seem to relieve my discomfort. I got out and realized my contractions were about four minutes apart and too painful at that point for me to walk through. I could still talk through them.
We turned on the Olympics, and I spent some time laboring on my hands and knees using my birth ball and our sofa edge for support. I knew I hadn't eaten in awhile, so I asked Don for a peanut butter sandwich.

Related: Labor and Birth Positions for Plus Size Women
At 3:37, my mom texted me and said she couldn't sleep. That woman had spidey senses! A little after four in the morning, I was vocalizing each contraction and felt that I was in enough pain to possibly be in active labor at that point (if only I knew how much worse it was going to get). My contractions were about four minutes apart.
We decided to go to labor and delivery.
Being in the car was torturous. Thanks to baby's positioning, a lot of my contractions were felt strongest in my lower back and every pothole in the road was torturous.
In labor and delivery, they triaged me quickly into an evaluation room and got me on a fetal monitor. I was positive we were staying, but when the midwife on duty evaluated me, I was shocked and disappointed to find out I was only 80% effaced and still maybe a centimeter and a half dilated.
I felt like I wanted to cry. If it was this painful and my body had barely (in my frame of mind at the time) done any work, how much worse was it going to get?
The midwife gave me another hour on the monitor, but I had no progress and she offered me a shot of morphine before sending us home around six in the morning. I rejected the morphine, so she told me to take two Benadryl at home and try to get some sleep.
Once home, I went straight back to the bathtub and Don brought me the Benadryl and a Tylenol. The tub was not soothing my back labor pain very much, so I got out and got into bed with Don.
He applied pressure to my lower back with his fist, which helped a little, but my contractions were still too intense to sleep much. I napped a little in between them, but not much.
Around 7:30, they were too strong to stay in bed, so I went back into the bath.
Laboring in the bath for maybe two hours, I called my mom at some point. I had to mute myself when contractions came because I knew I didn’t sound very good. I had planned a plus size natural birth from the beginning. So I was trying to mentally talk myself into believing that I could handle the pain for just a few seconds at a time.
I got back out of the bath and made my way back through the house, stopping twice for contractions, to get back into bed.
Though I had read several books about natural birth and watched some births online, I had not taken any classes. Don could tell I wasn’t managing my pain very well. He helped me breathe through contractions by telling me when to inhale and exhale. That helped me manage them enough to nap for short spurts in between them.
Around 9:30 that morning, they hurt too badly for me to stay lying down. I would jump up every time I felt one coming on. I'd grab onto one of the posts of our four poster bed, and bear down while having the contraction.
I asked Don to tell me when I had only thirty seconds left in the contraction, twenty seconds, and so on, and I got through them that way. When the pain intensified, I went into the bathroom and threw up.
By 11:30 that morning, I had been laboring after being sent home for over five hours. We decided to go back to the hospital. I went back through admissions and wrote on my paperwork for the reason for my visit: “I AM IN LABOR AND I WANT THIS BABY OUT.”
Related: Do I Need A Doula?
They stuck me back on the monitor. A new midwife from my practice named Megan was on duty, and she checked me. Sadly, I was still only two centimeters dilated after all those hours. I felt like I wanted to cry and had never heard such bad news in my life. So I was really starting to believe I could not achieve a natural, unaugmented birth.
I had gone for so many hours and only achieved another half centimeter of dilation. Megan tried to encourage me as I started saying really incoherent things about how my body was deficient. She started to tell me that I was more effaced and that I had made some progress. Megan wanted to send us back home but told me I could have an hour to try to progress. She let me walk the halls to help move things along.
When she checked me again, I had made zero progress. She brought up me going back home again, and I had to fight back tears while explaining that I could not imagine getting back in the car for another trip home. She gave me another hour and brought me a birth ball, which I sat on through contractions.
At the end of the hour, they put me on the fetal monitor, which was unbearable because I had to be on my back. Frequently I'd jumping up off the bed to throw up in the sink, and leaning on the sink counter through contractions. I wanted to labor in the shower, but since I was stuck in triage, one was not available. Instead, I ran my hand under the cold sink water during contractions.
When Megan checked me again, I had still made no more progress.
I asked about a Pitocin drip, but she reminded me I asked to avoid Pitocin. She told me I could have a bag of saline before she discharged me, to help my body energize and hopefully progress.
It was SO HOT in the triage room. I was sweating buckets and throwing up all afternoon with only some sips of water here and there. Don had been putting damp paper towels on my forehead and neck the entire time because they would get boiling hot against my skin in just ten or fifteen seconds.
A nurse came to administer the IV fluids, which probably bought us another hour of time in triage. I didn’t realize it then because my midwife was NOT my favorite person at that point. Yet, she probably did do this on purpose to try to give me some more time in the hospital to progress. Megan told me that if I could make any significant progress, she would admit me.
The saline seemed to help my body relax a little, and I took a short nap in between my contractions. Megan found that I had dilated to 3.5 centimeters on the saline drip. She needed 4 to admit me, but she fudged it so that I could be admitted. WRINGING her hands with gratitude, I was so relieved.
I think that once I was admitted and transferred to labor and delivery, the nerves and mental blocks that were impeding my body’s progress went away. We moved over to the labor and delivery suite around 5:30 pm.
I had at this point been in labor for nearly nineteen hours.
In labor and delivery, I continued to labor over the room’s sink counter and run my hands and arms under the faucet during contractions.
Megan recommended a dose of fentanyl to help me rest for the real work ahead, and another bag of saline. I was still set on my natural labor. She said my body really needed rest, that the fentanyl could help me avoid a c-section. They would monitor the baby while they put me on a thirty-minute drip. I agreed.
The fentanyl did take the edge off, and I napped for a half hour.
After the drip finished, I requested to be unhooked from the IV pole and went to the bathroom. When I sat down, my water broke. Don called our nurse who checked me and said I was dilated to a six. I went from a 3.5 to a six in about an hour. It was 6:37.
I labored on my hands and knees in the bed for a while. As well as on my hands and knees against the foot of the bed, and then on the birth ball. I felt like my body wanted to start pushing pretty early on after my water broke. Don tells me that around seven, I stopped vocalizing my contractions, which was probably a big relief for him after listening to me scream like a banshee all day.
I think this was when my body started transitioning.
I just let it do its thing during contractions, and tried to rest and relax completely while waiting for the next set of contractions to come. They were right on top of each other, so Megan came in and put me back on the fetal monitor.
I tolerated this for a few minutes before announcing to Don that my pain was unbearable and that I needed to get in the shower. I undressed the rest of the way out of my gown and unhooked myself from the monitor. While headed to the shower, my nurse showed back up and told me that Megan needed me to stay on the monitor for five more minutes. Then she promised I could labor in the shower.
I asked them to figure out how to get the monitor to work while I was on my hands and knees in the bed. So the nurse stood and held it on my stomach while strong waves and the urge for my body to push continued to rush over me. The nurse noticed I was straining to push and called Megan.
I barely even noticed when she checked my dilation again as I was fully focused on pushing. I was still begging her to let me get into the shower when she announced I was at 9 centimeters and almost there. She urged me to let my body work, but not to force it just because I was about to tear my cervix with the force of my pushing. That should have been terrifying to hear, but honestly, I couldn’t care about anything at that moment except getting the baby out.
Related: Grey’s Anatomy Encourages Having An Orgasm While In Labor
I stayed on all fours on the bed and gripped the headboard to push. It felt great to push through the contractions. Knowing I was at 9 centimeters reenergized me and gave me the confidence I needed to see it through. I was asking Megan how much longer she thought this would go on, and she just laughed and said if she could predict that, she’d be a millionaire.
Don ran ice up and down my back because I was very hot and sweaty. I was gripping his hands and the headboard and pushing spontaneously without coaching from Megan. She did say encouraging things to me as I worked, which was awesome because I tend to do well with verbal praise. Eventually, she called for a delivery cart, and Don tells me she gowned up, and got ready to catch Baby.
She asked me how I wanted to get him once I delivered because I was still on all fours. I somehow was still cohesive enough to tell her that I would flip over after she caught him and take him on my chest.
The most difficult part for me was when his head started to crown.
It hurt like nothing I’ve ever experienced. While I had been pretty quiet since I transitioned, I know I was screaming that it hurt. It must have been pretty incoherent. My midwife and nurse had a casual conversation about how primal I sounded and that I must be close now.
They could see a head of hair, and to keep going. The midwife helped me stretch around baby’s head, which hurt like the devil. She kept telling me I was being strong and doing a great job. As his head continued to crown, I heard a second nurse that was brought in say, “that’s a BIG baby,” and I stopped everything to shout, “what did you say?!” But like I said, I did predict he would be big.
I felt a huge sense of relief after I pushed his head out. He was born in one more push. While it felt like hours, I was told I pushed for twelve minutes after the midwife and nurses arrived.
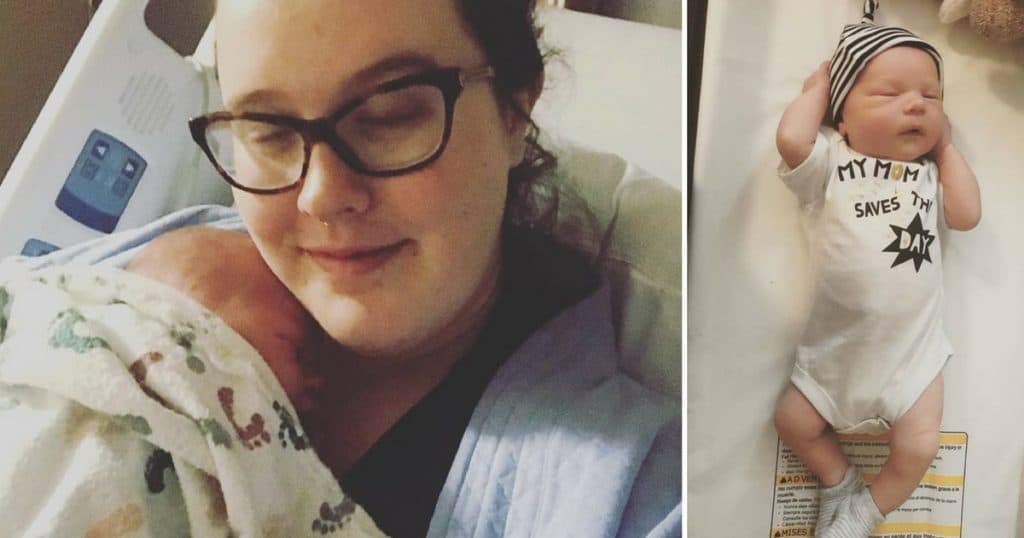
I flipped over from all fours and took my baby on my chest. He was so beautiful.
He was quiet as they toweled him down and staring up at me, not screaming like in the movies. I felt my heart burst as we looked at each other. The whole universe just exploded into a million pieces and got put back together with my baby boy at the center of it all. I kept looking at him and then to his daddy, who was speechless for maybe the first time in his life. We couldn't stop smiling at each other.

The nurses finished toweling and suctioning him. They hooked me up to a little bit of Pitocin to help me deliver the placenta. I also consented to some Demerol for pain management as the baby was out.
They weighed and assessed my son after the cord stopped pulsing and his dad cut it. I delivered the placenta, and Megan checked me for tears. I had one small periurethral tear. She did not feel the need to stitch because it would heal on its own.
Baby Everett scored a 9 on his APGAR assessment and was 9 pounds, 8 ounces, and 21 inches long. Born at 8:02 pm after over twenty hours of labor.

After all the uncertainty around becoming a parent, and the anxiety over whether or not he would be healthy and could be delivered naturally, it was amazing how everything just fell right into place.
I can’t imagine my life without him, and I’m so proud of myself for getting the birth experience I wanted. I definitely know that I will never be down on myself about my body again.
My body is a masterpiece after what it did to get my son here safely.
I’m very thankful for Don and my birth team for encouraging me to stick with my plan for the most part. They believed in me to get the job done. It might not have been a perfect journey, but it was beautiful for bringing my perfect son.
- Will My Baby Bump Show if I'm Overweight? - September 14, 2025
- Plus Size Maternity Pose Guide: 25+ Confidence-Boosting Poses - May 26, 2025
- Plus Size Pregnancy Confessions: We Listen and We Don't Judge - December 15, 2024